December 23, 2020
EndoRotor System is used to resect and remove necrotic (dead) tissue for patients with walled-off pancreatic necrosis (WOPN), a potentially deadly condition that can occur several weeks after an episode of severe acute pancreatitis, often requiring tissue removal.
“This device has shown its potential to provide a minimally invasive way to remove harmful necrotic pancreatic tissue in patients with walled-off pancreatic necrosis, which occurs in about 15 percent of patients with severe pancreatitis,” said Charles Viviano, M.D., Ph.D., acting director of the Reproductive, Gastro-Renal, Urological, General Hospital Device and Human Factors Office in the FDA’s Center for Devices and Radiological Health. “Currently, in order to remove dead tissue from a patient’s necrotic pancreatic cavity, health care providers need to perform an invasive surgery or use other endoscopic tools not specifically indicated to treat this condition. With today’s marketing authorization, patients with walled-off pancreatic necrosis now have a new treatment option.”
Pancreatitis occurs when digestive enzymes and inflammation cause cellular damage or tissue death. Necrotizing pancreatitis occurs when part of the pancreas dies because of inflammation or injury. After several weeks, the area of necrosis may form a walled off cavity and become what is called walled-off pancreatic necrosis. It is necessary to remove the dead tissue if it becomes symptomatic, such as worsening pain, causing infection which can lead to sepsis, or resulting in an obstruction to the intestines.
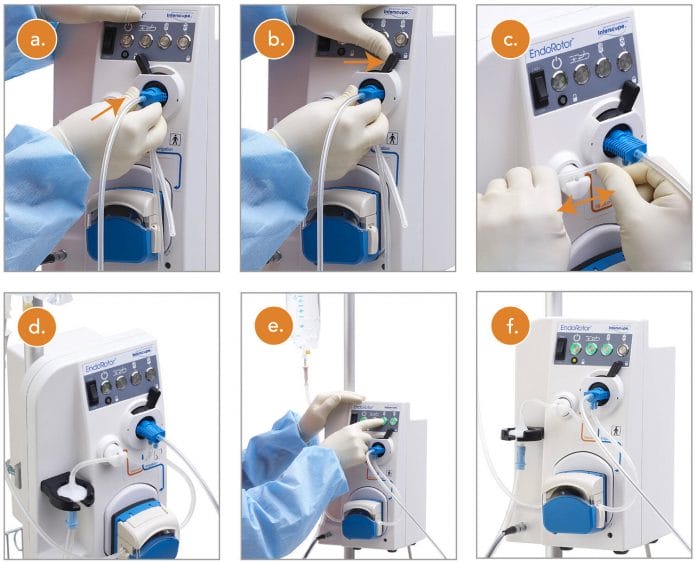
The EndoRotor System includes a power console, foot control, specimen trap and single-use catheter, and is used in a procedure called direct endoscopic necrosectomy that broadly consists of two steps. First, the user creates a portal, typically using a metallic stent, between the stomach and the necrotic cavity in the pancreas. This portal accommodates a standard endoscope—a flexible tube with a light and camera attached to aid in viewing the procedure. Second, the user places the EndoRotor through the working channel of the endoscope to cut and remove the necrotized tissue.
The FDA assessed the safety and effectiveness of the EndoRotor System in a trial with 30 subjects (23 enrolled in the U.S.) with walled-off pancreatic necrosis who were indicated to undergo a direct endoscopic necrosectomy. Study subjects were treated using the EndoRotor System during the procedure. Subjects often required multiple procedures, for a total of 63 direct endoscopic necrosectomies with the EndoRotor System to remove necrotic debris from the pancreatic cavity. This averaged 2.1 procedures per subject. Clinicians determined how many treatments a subject had based on whether symptoms—such as infected necrosis, fever, sepsis or pain—persisted after each procedure.
The device’s effectiveness was studied by how well it cleared necrotic tissue from the subject’s pancreas. The amount of necrotic tissue in each subject’s pancreas was measured during a computerized tomography scan with contrast before the procedure and compared to a follow up CT scan, endoscopy or MRI 14 to 28 days after the last procedure. For subjects undergoing procedures with the EndoRotor System, there was an average of 85% reduction in the amount of necrotic tissue, with half of the subjects having 98.5% clearance of their necrotic tissue.
In the clinical trial, three subjects experienced procedure-related serious adverse events (a 10% complication rate). Two of these subjects experienced gastrointestinal bleeding. The third subject experienced a pneumoperitoneum (air leaking from the pancreatic cavity into the abdominal cavity) and later died after suffering from sepsis and multi-organ system failure caused by massive collections of infected pancreatic necrosis.
Other serious adverse events recorded in the clinical trial, deemed to be due to the patient’s underlying condition and not related to the device or procedure, included hematemesis (vomiting of blood), deep vein thrombosis (blood clots) and pancreatitis.
The EndoRotor System should not be used in patients with known or suspected pancreatic cancer per the assessment of the treating physician. The FDA is requiring a boxed warning to emphasize this important point. The FDA is aware of a patient death (outside of the U.S.) from pancreatic cancer three months after having necrotic pancreatic tissue removed with the EndoRotor System. This patient did not have a diagnosis of pancreatic cancer prior to treatment, although the patient’s outcome is believed to be unrelated to the device or procedure.
The EndoRotor System should only be used in patients following other procedures to drain the walled-off pancreatic necrosis.
The EndoRotor System should not be used in patients with walled-off necrosis who have a documented pseudoaneurysm (when a blood vessel wall is injured and the leaking blood collects in the surrounding tissue) greater than 1 cm within the cavity or with intervening gastric varices (swollen veins in stomach) or unavoidable blood vessels within the access tract; or in patients with known or suspected pancreatic cancer.
The FDA reviewed the EndoRotor System through the De Novo premarket review pathway, a regulatory pathway for some low- to moderate-risk devices that are novel and for which there is no legally marketed predicate device to which the device can claim substantial equivalence.
The FDA granted marketing authorization of the EndoRotor System to Interscope, Incorporated.