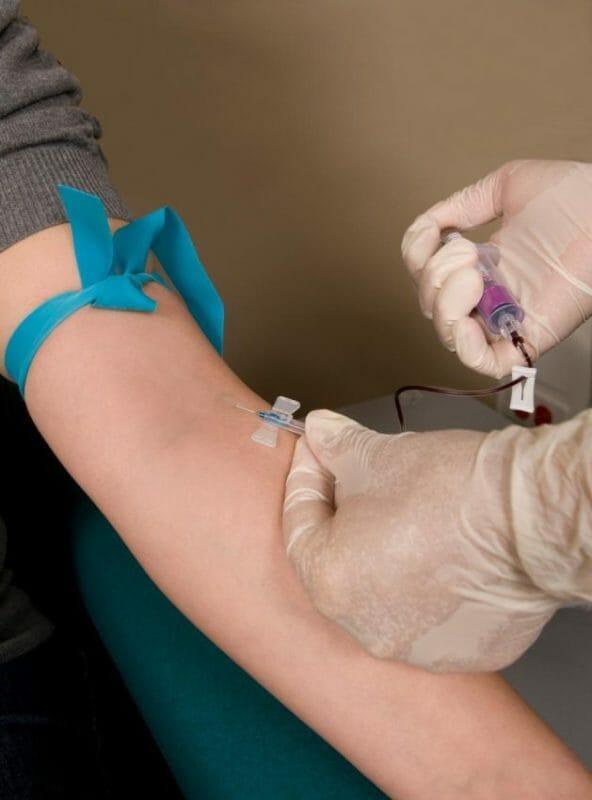
Phlebotomists draw blood from patients for various blood tests. These medical professionals work in hospitals, doctor’s offices, and surgical centers, among many other medical facilities. Unfortunately, mistakes happen frequently in the medical community, putting patients’ lives in danger. Phlebotomists must ensure they are not making common mistakes that could put their patients and job at risk.
Four Common Mistakes Phlebotomists Should Avoid
Phlebotomists have a critical job and must focus on their work to ensure proper practices. The field of phlebotomy is ever-widening, leading to advances that allow for greater patient comfort and precision. The following are some top mistakes phlebotomists must avoid in their day-to-day work in the medical community.
Improper Balance of the Centrifuge Machine
Proper balance in the centrifuge machine is critical. Improper balance leads to problems with blood samples, including hemolysis, which is the destruction of red blood cells. Hemolysis occurs when the tube vibrates violently inside its holding space. Glass tubes can also break as a result of improper balance. The phlebotomist must balance the machine by placing tubes across from one another. Balance the tubes carefully to avoid these problems and prevent job loss.
Forgetting to Verify Patient Information
Another mistake phlebotomists make is failing to verify patient information. Verifying the patient is extremely important. Phlebotomists must not get patients confused by labeling blood vials incorrectly or drawing the wrong amounts of blood from patients. Always check the wristband and order. Verify the patient’s name and date of birth before proceeding. Verification is a critical part of carrying out the work of a phlebotomist.
Improper Vein Selection
One of the top mistakes phlebotomists make, especially those new to the career, is selecting the wrong vein. Phlebotomists often try to go for the largest vein, but this is not always the best course of action. Phlebotomists cannot always see the patient’s veins but should be able to feel them. Choose a vein that feels soft and bounces. These veins are more likely to respond well and offer a steady flow of blood. Phlebotomists should ask their patients where they normally get blood drawn from.
Improper Angle
Another mistake phlebotomists make is going in the vein at the wrong angle. The most appropriate angle is 15 degrees for all superficial veins and 30 for deeper veins. Going in at the wrong angle could mean the vein does not release any blood. Going in too far could also lead to the phlebotomist going through the vein and hitting a nerve, causing great pain for the patient. It takes practice to perfect the right angle. Learning how to know when you have entered a vein is critical. You will feel a slight release when entering the vein.
Proper Training Is a Must
To avoid these mistakes, individuals must seek proper training to ensure they know the protocol to follow when drawing blood and preparing samples. It is also essential phlebotomists follow their training. Paying attention and preparing in advance with the right tools will ensure mistakes are avoided.
Phlebotomists are integral to the medical community and provide a service that ensures patients get the safe blood tests they require for diagnosis. Blood testing is critical for patient care and uncovers many signs of disease. When carried out appropriately, phlebotomists keep their patients safe and comfortable. With proper protocol, these medical professionals will not run into problems.