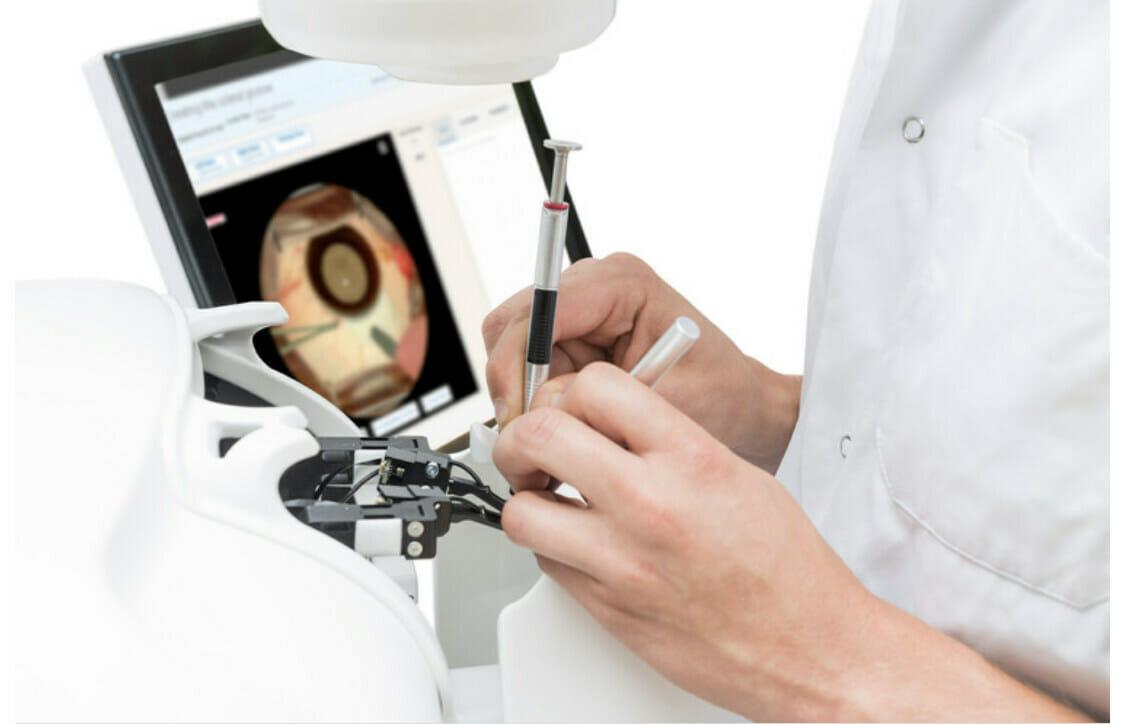
HelpMeSee has announced the launch of its next-generation simulation-based training for phacoemulsification. With instructor-led sessions and haptic feedback, this first-of-its-kind eye surgery training creates an immersive experience with the look and feel of surgery in a human eye, without risks to patient safety. Today, more than 100 million people are blind or visually impaired due to untreated cataract and a lack of access to care.
“With an aging population worldwide, the need for more surgeons trained to perform cataract surgery is great. As we work to fight global cataract blindness, we are thrilled to launch HelpMeSee’s simulation-based training for phacoemulsification,” said Saro Jahani, president and CEO. “This instructor-led training offers the most versatile eye surgery simulator in the world. It provides a less experienced ophthalmologist the opportunity to practice surgery until he or she gets it right, and a more experienced ophthalmologist the opportunity to practice until he or she simply cannot get it wrong.”
Teaching the most modern techniques in cataract surgery today, HelpMeSee’s innovative, instructor-led training for phacoemulsification offers:
- High-fidelity haptics that allow a trainee to feel the sensations of surgery on a real eye and develop muscle memory for dealing with real tissues in surgery
- One-on-one coaching from a skilled surgeon and system-delivered cues that guide a trainee, and can be gradually removed to allow the trainee to make and correct mistakes.
- A critical bridge to live surgery, allowing a trainee to be fully immersed in the surgical experience over several days, with the ability to develop proficiency without risk to the safety of a patient
“HelpMeSee has a beautiful mission – to cure blindness – and an approach to simulation-based training that delivers a unique, immersive experience,” said Tristan Bourcier, ophthalmic surgeon and professor of ophthalmology at Strasbourg University Hospital in France. “The training intersects three key things: an instructor, who is a trained and experienced surgeon, that is coaching you every step of the way; a powerful simulator, and an eBook that is rich in assets for learning. The quality of the images and the haptic feedback creates a combination that is the dream team for anyone learning modern cataract surgery.”
“At Columbia University Irving Medical Center, we have integrated HelpMeSee’s simulation-based training into our overall curriculum for our residents,” said Royce W.S. Chen, MD and associate professor of ophthalmology at Columbia University Medical Center. “Their model of an instructor-led course of concentrated, high-fidelity simulation training represents a paradigm shift in ophthalmic education that will make our residents stronger surgeons.”
“For our team at Aravind, the HelpMeSee simulation-based training has helped in better surgical training to significantly minimize the surgical complications, thereby improving the quality of patient care we provide through our residents,” said Dr. Ravindran Ravilla, chairman and director of quality, Aravind Eye Care System in India.
“For residents and fellows in training and ophthalmologists, this training provides a unique opportunity to learn a new surgery and refine skills in just days,” said Van Lansingh, chief medical officer of HelpMeSee. “As the only training of its kind that is instructor-led and includes high-fidelity haptics, the training provides unlimited opportunities for trainees to experience eye surgery, with a laser focus on building strong skills and instilling the confidence live surgery requires.”
The addition of training for phacoemulsification complements HelpMeSee’s portfolio of training offerings, which includes manual small-incision cataract surgery (MSICS), cataract complications simulation and corneal and scleral suturing, which constitute a major portion of surgical procedures needed to deal with preventable blindness. The training is targeted to active surgeons seeking additional procedural/task surgical skills, surgeons opening a practice after graduating, mission surgeons, and surgeons returning after time away from live surgery.
Proceeds from the purchase of each training course will be used to further the nonprofit’s mission to eradicate cataract blindness in the world, in support of training that restores the gift of sight. Since 2010, HMS’s philanthropic efforts to train and support cataract surgeons and patients have enabled more than 265,000 sight-restoring procedures.