Masimo (NASDAQ: MASI) today announced the findings of a prospective study published in the British Journal of Neurosurgery in which Dr. Ankita Dey and colleagues at institutions in Bathinda and Pondicherry, India evaluated the use of noninvasive, continuous Masimo PVi®, as part of goal-directed fluid therapy (GDFT), to guide intraoperative fluid administration during neurosurgery – the first study to evaluate PVi in this surgical scenario – by comparing it to a parameter obtained invasively, stroke volume variation (SVV). The researchers concluded that “PVi and SVV are equally effective for guiding intraoperative goal-directed fluid therapy in adult neurosurgical patients scheduled for elective craniotomy for supratentorial brain tumors. However, PVi, being a noninvasive parameter, may be preferable.”1
Noting the value of GDFT for neurosurgical patients in particular, but that most of the dynamic parameters traditionally used to guide GDFT, such as SVV, are invasive, requiring the use of an intra-arterial catheter (an arterial line, or “A-line”), which is associated with a variety of complications, the researchers sought to determine whether a noninvasive parameter, PVi, whose measurements are derived from the photoplethysmographic waveform, might serve as a reliable predictor of fluid responsiveness in such a population. PVi, or pleth variability index, is a measure of the variations in perfusion index over the respiratory cycle, and is indicated as a noninvasive, dynamic indicator of fluid responsiveness in select populations of mechanically ventilated adult patients.
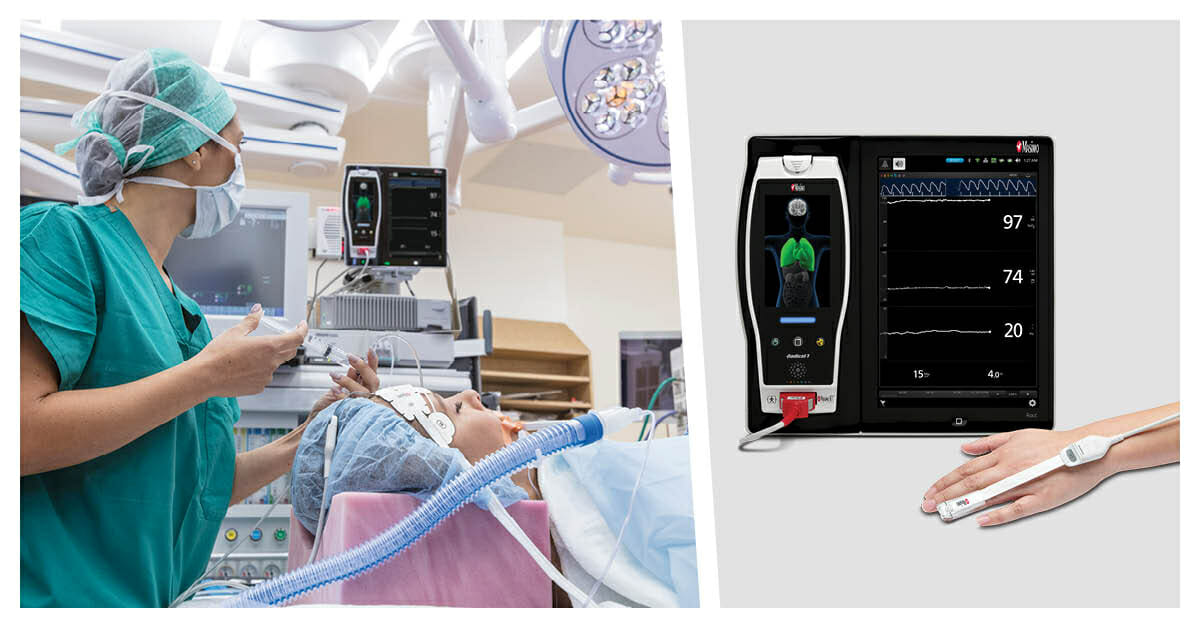
To test their hypothesis, the researchers randomly divided 60 adult patients undergoing elective craniotomy into two groups: one whose intraoperative fluid administration was guided by PVi (n=29) and the other, by SVV (n=31). In the PVi group, patients were monitored using Masimo Radical-7® Pulse CO-Oximeters® with noninvasive pulse oximetry fingertip sensors. In the SVV group, SVV was invasively measured using an Edwards Lifesciences Vigileo/FloTrac device connected to a cannulated radial artery. The researchers compared the total amount of intravenous fluid administered during surgery, as well as serum lactate and serum creatinine levels at pre-determined time points, the brain relaxation score at dural opening and closure, and correlation between PVi and SVV values. They also compared duration of mechanical ventilation and length of hospital stay.
As noted in the table below, the researchers found that the volume of fluid administered intraoperatively was significantly higher in the SVV group. The other parameters and outcomes they measured were comparable between the two groups: serum lactate, serum creatinine, brain relaxation score, duration of mechanical ventilation, and length of hospital stay, as noted below. The researchers also observed “a moderate to strong correlation between SVV and PVi at corresponding points of time during the intraoperative period. This suggests that PVi, derived noninvasively from the pulse oximetry waveform, is a reliable indicator of fluid responsiveness.”
|
Outcome |
PVi group |
SVV group |
p-Value |
|
Volume of fluid administered |
2139.3 ± 898.6 mL (mean) |
3208.3 ± 1836.2 mL (mean) |
0.005 |
|
Serum lactate level, over time |
Ranging from 1.59 ± 0.91 to 2.73 ± 1.18 |
Ranging from 1.79 ± 0.97 to 2.44 ± 0.88 |
Ranging from 0.55 to 0.82 |
|
Serum creatinine level, over time |
Ranging from 0.64 ± 0.14 to 0.66 ± 0.15 mg/dL |
Ranging from 0.64 ± 0.17 to 0.71 ± 0.21 mg/dL |
Ranging from 0.23 to 0.86 |
|
Brain relaxation score |
2 (1-3) at dural opening, 2 (12) at dural closing (median) |
2 (1-4) at dural opening and closing (median) |
0.49 (opening) 0.33 (closing) |
|
Duration of mechanical ventilation |
19.09 ± 15.9 hours (mean)
|
27.9 ± 15.9 hours (mean) |
0.1 |
|
Length of hospital stay |
12.6 ± 19.26 days (mean) |
16.4 ± 26.8 days (mean) |
0.53 |
The researchers concluded, “Based on the findings of our study, we conclude that PVi and SVV are equally effective for guiding intraoperative goal directed fluid therapy in adult neurosurgical patients scheduled for elective craniotomy for supratentorial brain tumors. However, PVi, being a noninvasive parameter, may be preferable.” They continued, “The two groups in our study were comparable with respect to serum creatinine and serum lactate measured at predetermined time points intraoperatively and post operatively. The two groups were also comparable with respect to brain relaxation scores at dural opening and dural closure. There was moderate to strong correlation between SVV and PVi at corresponding time points intraoperatively. The duration of mechanical ventilation and the length of hospital stay was also comparable between the two groups.”
Joe Kiani, Founder and CEO of Masimo, said, “We introduced PVi in 2007. It was the first and still is the only noninvasive way of measuring fluid responsiveness in mechanically ventilated patients at a fraction of the cost of invasive methods and without risk of invasive procedures to the patient. Since then, over 100 studies have shown that PVi or PVi in combination with our noninvasive hemoglobin technology, SpHb®, has made a tremendous contribution to patient care.2 This latest study adds to the evidence that PVi can be used to help clinicians manage the fluid levels of their patients without invasive catheters.”
In the US, PVi is FDA 510(k) cleared as a noninvasive dynamic indicator of fluid responsiveness in select populations of mechanically ventilated adult patients. Accuracy of PVi in predicting fluid responsiveness is variable and influenced by numerous patient, procedure and device related factors. PVi measures the variation in the plethysmography amplitude but does not provide measurements of stroke volume or cardiac output. Fluid management decisions should be based on a complete assessment of the patient’s condition and should not be based solely on PVi.
References
- Dey A, Bidkar PU, Swaminathan S, Kumari M, Joy JJ, Balasubramanian M, Bhimsaria S. Comparison of two techniques of goal-directed fluid therapy in elective neurosurgical patients – a randomized controlled study. Br J Neuosurgery. 3 Feb 2023. DOI: 10.1080/02688697.2023.2173722/
- Published clinical studies on PVi can be found on our website at https://www.masimo.com.
- Published clinical studies on pulse oximetry and the benefits of Masimo SET® can be found on our website at https://www.masimo.com. Comparative studies include independent and objective studies which are comprised of abstracts presented at scientific meetings and peer-reviewed journal articles.
- Castillo A et al. Prevention of Retinopathy of Prematurity in Preterm Infants through Changes in Clinical Practice and SpO2 Technology. Acta Paediatr. 2011 Feb;100(2):188-92.
- de-Wahl Granelli A et al. Impact of pulse oximetry screening on the detection of duct dependent congenital heart disease: a Swedish prospective screening study in 39,821 newborns. BMJ. 2009;Jan 8;338.
- Taenzer A et al. Impact of pulse oximetry surveillance on rescue events and intensive care unit transfers: a before-and-after concurrence study. Anesthesiology. 2010:112(2):282-287.
- Taenzer A et al. Postoperative Monitoring – The Dartmouth Experience. Anesthesia Patient Safety Foundation Newsletter. Spring-Summer 2012.
- McGrath S et al. Surveillance Monitoring Management for General Care Units: Strategy, Design, and Implementation. The Joint Commission Journal on Quality and Patient Safety. 2016 Jul;42(7):293-302.
- McGrath S et al. Inpatient Respiratory Arrest Associated With Sedative and Analgesic Medications: Impact of Continuous Monitoring on Patient Mortality and Severe Morbidity. J Patient Saf. 2020 14 Mar. DOI: 10.1097/PTS.0000000000000696.
- Estimate: Masimo data on file.
- https://health.usnews.com/health-care/best-hospitals/articles/best-hospitals-honor-roll-and-overview.